

 |
Top of page
There are two main types of compartment syndrome: acute and chronic:
- Acute compartment syndrome occurs after a traumatic injury such as a car crash. The trauma causes a severe high pressure in the compartment which results in insufficient blood supply to muscles and nerves. Acute compartment syndrome is a medical emergency that requires surgery to correct. If untreated, the lack of blood supply leads to permanent muscle and nerve damage and can result in the loss of function of the limb.
- Chronic exertional compartment syndrome is an exercise-induced condition in which the pressure in the muscles increases to extreme levels during exercise. The pressure creates a decrease in blood flow to the affected area which leads to a deprivation of oxygen to the muscles. The symptoms are a sensation of extreme tightness in the affected muscles followed by a burning sensation if exercise is continued. Chronic exertional compartment syndrome usually occurs in athletes who participate in repetitive impact sports such as running.
Top of page
Acute compartment syndrome

The first signs of compartment syndrome are numbness, tingling and paresthesia. Loss of function and decreased pulses or pulselessness, however, are late signs.
- Pain is often reported early and almost universally. The description is usually of deep, constant, and poorly localized pain out of proportion with the findings on physical examination (often incorrectly described as pain out of proportion to the injury). The pain is aggravated by passively stretching the muscle group within the compartment or actively flexing it (though this finding is not specific to compartment syndrome alone) and is not relieved by analgesia up to and including morphine.
- Paresthesia (altered sensation e.g., "pins & needles") in the cutaneous nerves of the affected compartment is another typical sign.
- Paralysis of the limb is usually a late finding. The compartment may also feel very tense and firm (pressure). Some find that their feet and even legs fall asleep. This is because compartment syndrome prevents adequate blood flow to the rest of the leg.
- A lack of pulse rarely occurs in patients, as pressures that cause compartment syndrome are often well below arterial pressures and pulse is only affected if the relevantartery is contained within the affected compartment.
- Tense and swollen shiny skin, sometimes with obvious bruising of the skin.
- Congestion of the digits with prolonged capillary refill time.
Chronic exertional compartment syndrome
The symptoms of chronic exertional compartment syndrome (CECS) are brought on by exercise and consist of a sensation of extreme tightness in the affected muscles followed by a painful burning sensation if exercise is continued. After exercise is ceased, the pressure in the compartment will decrease within a few minutes, relieving painful symptoms. Symptoms will occur at a certain threshold of exercise which varies from person to person but is rather consistent for a given individual and can range anywhere from 30 seconds of running to about 10–15 minutes of running. CECS most commonly occurs in the lower leg, with the anterior compartment being the most frequently affected compartment. Foot drop is a common symptom of CECS.
Top of page
Causes
Acute compartment syndrome
Because the fascia layer that defines the compartment does not stretch, a small amount of bleeding into the compartment, or swelling of the muscles within the compartment, can cause the pressure to rise greatly. Common causes of compartment syndrome include tibial or forearm fractures, ischemic reperfusion following injury, hemorrhage, vascular puncture, intravenous drug injection, casts, prolonged limb compression, crush injuries and burns. Less common causes include labor and delivery following uncomplicated births and csections. Compartment syndrome can also occur following surgery in the Lloyd-Davies lithotomy position, where the patient's legs are elevated for prolonged periods.
Chronic compartment syndrome
When compartment syndrome is caused by repetitive use of the muscles, as in a cyclist, it is known as chronic compartment syndrome (CCS). This is usually not an emergency, but the loss of circulation can cause temporary or permanent damage to nearby nerves and muscles. The cause of compartment syndrome is due to excess pressure on or within the muscle compartments. This pressure can occur for many different reasons, many are due to injuries. Injuries cause the swelling of tissue. The swelling of the tissue forces pressure upon the muscle compartments, which has a limited volume. Due to this pressure, the venules and lymphatic vessels that drain the muscle compartments are compressed, and are prevented from draining. As arterial inflow continues while outflow is decreased, the pressure builds up in the muscle compartments. This pressure will eventually decrease the amount of blood flow over the capillary bed, causing the tissue to become ischaemic. The tissues will release factors and will lead to the formation of edema.
Chronic exertional compartment syndrome
Complementary to chronic compartment syndrome is another subset known as chronic exertional compartment syndrome CECS, often called exercise induced compartment syndrome EICS. CECS of the leg is a condition caused by exercise which results in increase tissue pressure within a limited fibro – osseous compartment – muscle size may increase by up to 20% during exercise. When this happens pressure builds up in the tissues and muscles causing tissueischemia. An increase in muscle weight will reduce the compartment volume of the surrounding fascial borders and resulting in an increase of intracompartmental pressure. An increase in the pressure of the tissue can cause fluid to exude into the small spaces between the tissue known as interstitial space, leading to a disruption of the micro-circulation of the leg. This condition occurs commonly in the lower leg and various other locations within the body, such as the foot or forearm. This is commonly seen in athletes who train rigorously in activities that involve constant repetitive actions or motions.
Symptoms involve numbness or a tingling sensation in the area most affected. Other signs and symptoms include pain described as aching, tightening, cramping, sharp, or stabbing. This pain can occur for months, and in some cases over a period of years, and may be relieved by rest. It also includes moderate weakness that can be a noticeable factor in the affected region. Chronic exertional compartment syndrome most commonly affects the anterior compartment of the leg, this can lead to problems with dorsiflexion of the ankle and the toes. The symptoms of CECS are often confused with more common injuries like shin splints and spinal stenosis. Treatment for chronic exertional compartment syndrome includes decreasing or subsiding exercising and activities, or cross training for athletes. In cases with severe intracompartmental pressures surgical treatment, a fasciotomy, is necessary.
Top of page
Diagnosis
Compartment syndrome is a clinical diagnosis made by a physician. It can be tested for by gauging the pressure within the muscle compartments. If the pressure is sufficiently high, a fasciotomy will be required to relieve the pressure. Various recommendations of the intracompartmental pressure are used with some sources quoting >30 mmHg as an indication for fasciotomy while others suggest a <30 mmHg difference between intracompartmental pressure and diastolic blood pressure. This latter measure may be more sensible in the light of recent advances in permissive hypotension, which allow patients to be kept hypotensive in resuscitation. It is now relatively easy to measure compartment and subcutaneous pressures using the pressure transducer modules (with a simple intravenous catheter and needle) that are attached to most modern anaesthetic machines. Most commonly compartment syndrome is diagnosed through a diagnosis of its underlying cause and not the condition itself. According to Blackman one of the tools to diagnose compartment syndrome is X-ray to show a tibia/fibula fracture, which when combined with numbness of the extremities is enough to confirm the presence of compartment syndrome.
Top of page
Treatment
Acute compartment syndrome
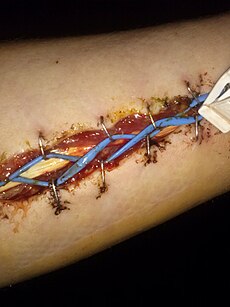
Acute compartment syndrome is a medical emergency requiring immediate surgical treatment, known as a fasciotomy, to allow the pressure to return to normal. Although only one compartment is affected, fasciotomy is done to release all compartments. For instance, if only the deep posterior compartment of a leg is affected, the treatment would be fasciotomy (with medial and lateral incisions) to release all compartments of the leg in question, namely the anterior, lateral, superficial posterior and deep posterior. An acute compartment syndrome has some distinct features such as swelling of the compartment due to inflammation and venous occlusion. Decompression of the nerve traversing the compartment might alleviate the symptoms.
Chronic compartment syndrome
Chronic compartment syndrome in the lower leg can be treated conservatively or surgically. Conservative treatment includes rest, anti-inflammatories, and manual decompression. Elevation of the affected limb in patients with compartment syndrome is contraindicated, as this leads to decreased vascular perfusion of the affected region. Ideally, the affected limb should be positioned at the level of the heart. The use of devices that apply external pressure to the area, such as splints, casts, and tight wound dressings, should be avoided. If symptoms persist after conservative treatment or if an individual does not wish to cease engaging in the physical activities which bring on symptoms, compartment syndrome can be treated by a surgery known as a fasciotomy. Surgery is the most effective treatment for compartment syndrome. Incisions are made in the affected muscle compartments so that they will decompress. This decompression will relieve the pressure on the venules and lymphatic vessels, and will increase bloodflow throughout the muscle. Left untreated, chronic compartment syndrome can develop into the acute syndrome and lead to permanent muscle and nerve damage.
Top of page
Complications
Failure to relieve the pressure can result in necrosis of tissue in that compartment, since capillary perfusion will fall leading to increasing oxygen deprivation of those tissues. This can cause Volkmann's contracture in affected limbs. As intercompartmental pressure rises during compartment syndrome, perfusion within the compartment is reduced leading to ischemia, which if left untreated, results in necrosis of nerves and muscles of the compartment. Rhabdomyolysis and subsequent renal failure are also possible complications.
Back to top
|
Page Content |


